Today’s post is, unfortunately, exposing me a little, but I think it’s necessary transparency. As a woman and someone who works in healthcare, I’m ashamed to say that I don’t know enough about Menopause as I should. I know it’s not good, but really, other than the basics, I don’t really understand a whole lot about Menopause. In this week’s article, I will be educating myself as much as I’m educating you. I hope you learn something as we go on this journey together. If you are currently going through Menopause yourself, this is the perfect article to send to your partner, family, or friend to help them understand what you’re currently going through, and later in the article, we’ll talk about how they can support you!
What is Menopause?
Firstly, menopause is a fact of life. It is not a disease. It is the natural, permanent cessation of menstruation that occurs in women as the number of eggs they have decreases (1,2). Menopause is reached if a woman has not had a period for over 12 months, as a result of a reduction in the natural sex hormones that stimulate the usual menstrual cycle. After this time, women are considered ‘post-menopausal’. This means that if you have not had a period due to other causes like PCOS, hormonal contraception, stress, weight loss, etc, this does not mean that you are going through menopause.
Quick Facts:
- The average age of menopause is 45-55 years old, although menopause can start before or after this time.
- 2-4% women worldwide experience menopause before 40 years. This is known as Early Menopause or Premature Ovarian Insufficiency (POI) (3).
- Roughly 75% of women experience Menopausal symptoms, with 25% of these women describing these symptoms as severe.
… A Bit on the Science of Menopause
When a woman is born, she has a set number of eggs that she possesses. These eggs are stored in the ovaries, and when she starts puberty, one by one, the eggs go through a cycle of maturation every month.
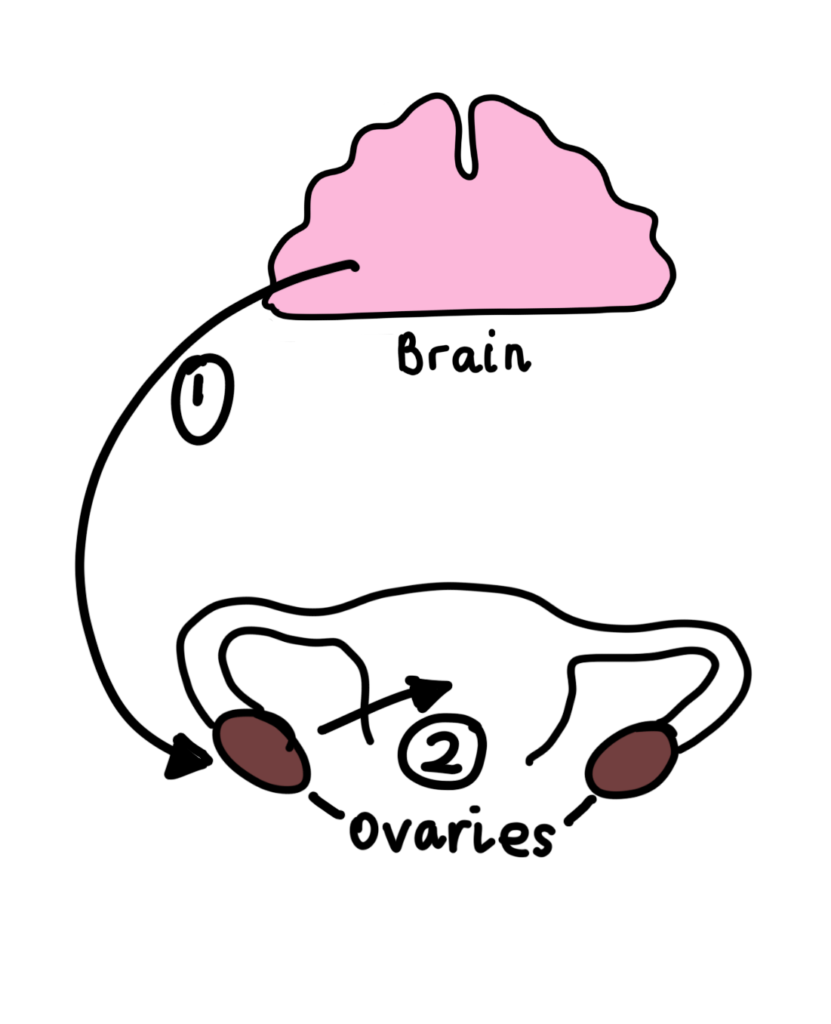
- During the menstrual cycle, the brain releases two main hormones called Follicular Stimulating Hormone (FSH) and Luteinising Hormone (LH) to stimulate one egg to become more mature. The egg is in a sac (follicle) which then produces oestrogen and progesterone, as well as other hormones, and releases this to the uterus to prepare the lining of the uterus (endometrium) for a possible pregnancy. If this pregnancy doesn’t occur, the lining sheds. The eggs are discarded from the body, the oestrogen and progesterone levels drop, and another cycle begins.
- As women get older, the number of eggs reduces with each menstrual cycle. Because the number of eggs reduces, the level of oestrogen and other hormones also reduces. Over time, this causes the endometrium to become thin and unable to prepare for pregnancy. This, in turn, means there is no menstruation (3).
- Low oestrogen causes a signal to be sent back to the brain, which triggers the release of more FSH and LH. Menopause is achieved when oestrogen levels are very low, and FSH and LH levels are high. Because this process can take months to years to be fully complete, we refer to this period of transition as being perimenopausal (4).
Figure 1 – Hormonal Release in the Reproductive System: This diagram shows the release of hormones to the brain [part 1] and how they stimulate the release of hormones to the uterus [part 2]. Created by Mojibola Orefuja.
Signs and Symptoms of Menopause
So now we know what Menopause is, how can we spot the signs of it? Below is a list of some of the symptoms that have been experienced by different women when going through menopause:
- Hot flashes – These are feelings of intense body heat which can last several minutes. Unfortunately, for some women, these symptoms can remain for 4-5 years. Some studies even suggest that Black and African American women experience hot flashes the most intensely and for the longest amount of time (4,5).
- Vaginal dryness, narrowing and shortening – As oestrogen reduces, its impact on the female reproductive system also reduces. This means that the maintenance of the vagina is affected. This results in symptoms of dryness, pain, redness, and difficulty with intercourse. These symptoms are common and can lead to other symptoms and problems like itching, burning, pain and infections (4).
- Mood changes, including increased depression and anxiety – Studies have shown that women experience intense depressive symptoms during perimenopause, and these feelings peak in late perimenopause (6). Studies also show that depressive symptoms may arise as a result of menopausal symptoms, due to the effect on quality of life (7).
- Sleep disturbances – While studies haven’t yet been able to confirm that the hormonal decline in menopause is linked to sleep disturbance, studies have shown that if an individual has prior sleep difficulties, this may decline and worsen during the perimenopausal period. This could be due to symptoms experienced in menopause, or be because of menopause itself (4, 8).
- Bone fractures and back pain – As with most hormones, oestrogen is involved in processes other than reproductive health. Oestrogen helps to maintain the strength of our bones by stopping our body from breaking down our bones for calcium. With lower oestrogen levels, this process of protecting our bones is significantly reduced, causing fragile and thin bones. This can lead to frequent bone and back pain (4).
Treatment
Treatment for Menopause can be split into 3 main groups:
- Hormonal medical treatments – Hormonal replacement therapies (HRT) are often offered to women with significant, intense symptoms that need management to reverse the effects. These are medication which have some form of oestrogen, progesterone or both inside them. It is important to note that these are offered with a full understanding of the risks they pose to heart health, and also with increasing your risk of breast cancer. These therapies are not given to women with a history of heart disease, breast cancer or family history of either of these conditions.
- Non-hormonal medical treatments – These are offered to women who can’t have hormonal therapies, but also to women with symptoms that are not severe, but would like intervention. These medications are usually tailored to balance the nervous system symptoms of menopause, like hot flashes. These have less significant complications and side effects, but you still need to know the risks before deciding on this option. Other non-hormonal treatments include things like calcium supplements to help with bone strength and supplements to help with sleep.
- Non-medical treatments – These are approaches like lifestyle advice, talking therapies, educational courses and herbal remedies. Herbal remedies are not regularly offered within the NHS.
How can you support someone going through menopause?
Firstly, you need to understand what’s happening. The symptoms above are not simple or easy symptoms to live with. They affect people quite intensely, and a little understanding goes a long way. Women are able to deal with the effects of menopause more easily if they know that those around them are supporting them through it (10). Another thing you can do is help them with their symptoms. If a woman is experiencing a hot flash and asking for the area to be cold for a short period of time, it is empathetic to accommodate her. Thank you for taking the time to read this article. Don’t stop here, though; do your research and learn more about what menopause really is.
References
- Peacock K, Carlson K, Ketvertis KM. Menopause [Internet]. StatPearls – NCBI Bookshelf. 2023. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507826/
- Davis S, Pinkerton J, Santoro N, Simoncini T. Menopause-Biology, consequences, supportive care, and therapeutic options. Cell. 2023 Sep 14;186(19):4038–58.
- Menopause: Whats causes it? [Internet]. NICE CKS. 2025. Available from: https://cks.nice.org.uk/topics/menopause/background-information/causes/
- Santoro N, Roeca C, Peters B, Neal-Perry G. The Menopause Transition: Signs, Symptoms, and Management Options. The Journal of Clinical Endocrinology & Metabolism. 2021 Jan;106(1):1–15.
- Avis N, Crawford S, Greendale G. Duration of Menopausal Vasomotor Symptoms Over the Menopause Transition. JAMA Internal Medicine. 2015 Apr;175(4):531–9.
- Bromberger JT, Kravitz HM, Chang Y f., Cyranowski JM, Brown C, Matthews KA. Major depression during and after the menopausal transition: Study of Women’s Health Across the Nation (SWAN). Psychological Medicine [Internet]. 2011 Feb 9;41(9):1879–88. Available from: https://www.cambridge.org/core/journals/psychological-medicine/article/abs/major-depression-during-and-after-the-menopausal-transition-study-of-womens-health-across-the-nation-swan/C1492885FCBF9B68C0990E70845F4DF4
- Avis NE, Crawford S, Stellato R, Longcope C. Longitudinal study of hormone levels and depression among women transitioning through menopause. Climacteric [Internet]. 2001 Jan 1;4(3):243–9. Available from: https://doi.org/10.1080/cmt.4.3.243.249
- Kravitz H, Ganz P, Bromberger J, Powell L, Sutton-Tyrell K, Meyer P. Share Favorites Permissions ARTICLES Sleep difficulty in women at midlife: a community survey of sleep and the menopausal transition. Menopause: The Journal of the Menopause Society. 2003 Jan;10(1):19–28.
- Strelow B, O’Laughlin D, Anderson T, Cyriac J, Buzzard J, Klindworth A. Menopause decoded: What’s happening and how to manage it. Journal of Primary Care & Community Health [Internet]. 2024 Jan 1;15:21501319241307460. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC11663262/
- Supporting someone through menopause [Internet]. NHS Inform. Available from: https://www.nhsinform.scot/healthy-living/womens-health/later-years-around-50-years-and-over/menopause-and-post-menopause-health/supporting-someone-through-the-menopause/
